If there is one experience that all women (of reproductive age) share across the planet, across cultures and borders, it is the menstrual cycle. While it is a natural process of the female body, some of the symptoms that accompany it can be unpleasant or even painful. Menstrual cramps are possibly the worst part of having your period, but there are some things you can do to ease the pain.

What are menstrual cramps?
Period pain is medically known as dysmenorrhoea. It does not affect all women equally – some women do not experience it at all; but for some women, it can prevent them from going about their regular lives. Over the years, several methods and ways have evolved to help women tackle this pain and provide period pain relief.
Period pain occurs when the uterus cramps or contracts, causing pain in the lower abdomen or pelvic region. For some women, the pain may radiate up the back or down into the legs.
Period pain is especially common in younger women and should ease as the woman gets older. However if you experience such severe pain that it interferes with your daily activities, you should consult a doctor.
What are the symptoms of period pain?
The primary symptom of period pain is pain in the pelvic region which starts before the onset of bleeding. It may go on for the duration of the period or only for the first 2-3 days.
The severity of the pain varies from one individual to another and can range from mild discomfort to debilitating. You may not always experience the same level of menstrual cramps, with some months being easier than others.
The other symptoms that accompany periods tend to be:
- Pain in the lower back
- Dizziness
- Nausea and vomiting
- Unexplained fatigue
- Migraines and headaches
- Gastrointestinal discomfort
Types of cramps
There are two types of period pain: primary and secondary dysmenorrhoea.
Primary dysmenorrhoea
Primary dysmenorrhoea is pain caused by your period. It cannot be attributed to any other underlying medical condition. This usually begins with the first period but often gets better with age.
It is believed that a chemical called prostaglandin causes period pain. This substance is secreted by the uterine lining to help it shed. To do this, it causes contractions of the uterus and the muscles of the pelvis. This contraction is responsible for the tight, heavy feeling in the pelvic area.
Prostaglandins constrict and compress the blood vessels in the uterus, reducing the normal blood supply. They are also responsible for the gastro discomfort and nausea associated with periods. The higher the level of prostaglandin in the body, the greater the severity of the symptoms.
Risk factors for primary dysmenorrhoea include:
- Heavy bleeding
- Obesity
- Periods beginning at a very young age
- Family history
- Drinking alcohol
- Prolonged periods
- Smoking
Secondary dysmenorrhoea
Secondary dysmenorrhoea is pain caused by medical problems. It is often diagnosed in women in their 30s or 40s. In this condition, the pain persists during the entire bleeding duration and also between periods. It may get worse over time.
The symptoms of secondary dysmenorrhoea include:
- Recent changes in period pain
- Irregularity of periods
- Pain and bleeding during intercourse
- Vaginal discharge
- Heavy periods
- A high fever during periods
- Difficulty going to the toilet
What is the difference between primary and secondary cramps?
Your medical practitioner is best suited to diagnose your period and provide you with period pain relief. Your doctor will ask questions about your symptoms, and menstrual cycle and, if necessary, conduct a physical examination.

Primary dysmenorrhoea can usually be diagnosed after a conversation and basic examination. To correctly diagnose secondary dysmenorrhea, you may need to undergo some tests, especially if you have debilitating pain and exhibit any other symptoms.
The tests usually include:
- Hysteroscopy
- Ultrasound scan of the pelvic region
- Laparoscopy
When are menstrual cramps considered normal?
The severity of pain experienced during periods varies on an individual basis. While some experience minimal discomfort, others have severe pain that can interfere with their daily activities. No one can know what your pain is like so it is only you who can decide what your ‘normal’ period pains are like and when something is not normal.

Period pain is more common in women in their 20s, but it usually lessens as you move into your 30s and 40s. Certain symptoms can help you decide if the pain is normal such as:
- Discomfort in the lower back, stomach and legs
- Nausea or vomiting
- Gastrointestinal discomfort, diarrhoea
- Pain that is present only for the first two days of the period
- Pain that dissipates when you take medication
- The pain does not interfere with daily living
When are menstrual cramps not considered normal?
If the pain and symptoms are different or more extreme than the cramps you usually experience, it may be caused by something else. Do note that the intensity or level of period pain can vary from one period to another.
Medically speaking, period pain that arises in the uterus muscles i.e. myometrium on the first two days of the period is normal. Pain that arises from the endometrium and persists for more than the first two days of the period is considered abnormal. If you experience the latter, your pain might be more severe than others and you might suffer from one of two conditions:
- Adenomyosis: When cells that usually form the lining of the uterus grow into the wall of the uterus
- Endometriosis: When cells of the inner lining of the uterus spread outside the uterus. This condition usually begins in the late teenage years.
Period pain relief: Hormonal therapy
Hormonal treatments tend to reduce menstrual cramps by thinning the uterine lining. This reduces the production and release of prostaglandins during your period thereby reducing the frequency and strength of uterine contractions. Your periods tend to become lighter and less frequent with hormonal treatments.
The forms of hormonal therapy available are:
- Certain combinations of oral contraceptives
- Other forms of contraceptives such as vaginal ring
- Long-term options such as injections and implants
- Hormone-secreting intra-uterine devices (IUDs)
Period pain relief: Medication
There is a wide range of medication available for menstrual cramps. The most widely recognized categories of medicines are:
Pain relievers
These medicines which are branded non-steroidal anti-inflammatory drugs (NSAIDs) are one of the primary forms of medications suggested for period pain. They work by halting the production of prostaglandins – the chemical that is most associated with period pain.
NSAIDs are most effective when they are taken just before (if you recognize the symptoms) the onset of pain or when the pain begins. The most common types that might be suggested by your medical practitioner are:
- Mefenamic acid (Ponstan)
- Ibuprofen (Advil, Rafen)
- Naproxen (Inza, Naprosyn)
If you have any of these existing conditions, NSAIDs may cause issues for you. It is best to consult your medical practitioner before self-medicating in this case.
- With existing symptoms of stomach ulcers and indigestion. For this reason, they are recommended to be taken only after food
- Allergic reaction to aspirin
- Suffering from asthma
- Problems related to the kidneys
It is best to consult your doctor or medical practitioner before you start a course of any new medication. If you feel NSAIDs are not for you, you could consider other pain relievers such as
paracetamol and aspirin. Stronger medication that has codeine is only available over the counter by the presentation of a medical prescription.
Oral contraceptive pill (OCP)
This is the second group of medications that is widely considered and recognized when it comes to menstrual pains and periods. It works differently than pain relievers and should only be taken after consulting your medical practitioner. Bear in mind the following:
- Ask for an OCP that has a higher ratio of progestogen than estrogen for higher efficacy
- Take OCPs only if you are planning to have a period every two to three months or not at all as they are known to severely alter your hormonal cycle
Your level of pain and current physical condition dictate the type of medication you should use. Do check with an expert if you are not sure.
Home remedies for period pain relief
Self-care measures which can easily be done at home are considered amongst the safest and easiest remedies for menstrual cramps. Some of the at-home measures that you can undertake are:
- Heat can reduce the cramping associated with periods. Use a heat pack, try lying down with a water bottle on your pelvis or abdomen, or take a warm shower. These methods can provide immediate relief from period pain.
- While you may not feel up to it, regular exercise during the month can reduce period pain. During your period, avoid anything strenuous and try going for a walk or doing a light session of stretching. This releases endorphins (natural feel-good hormones) that trigger the body’s supply of painkillers and can have a significant effect on period pain.
- Mental rest is just as important as physical rest. When you are stressed or mentally fatigued, you may feel the effects of menstrual cramps more severely than otherwise. A routine of meditation, self-care and exercise during the rest of the month can help reduce period pain over time.
- Smoking and drinking are known to aggravate pain associated with periods. Many people like to avoid stimulants like caffeine, alcohol or nicotine in the days leading up to the period.
- A gentle massage on your abdomen may help reduce pain. Some people like to mix soothing essential oils like lavender with coconut oil for this, but plain coconut oil is fine too. Apply a few drops and rub your hands in a circular motion over your stomach and abdomen. Doing this for a few minutes can increase circulation and reduce muscle cramps. Find out how to do a simple, soothing massage at home.

How do diet and nutritional supplementation provide period pain relief?
Diet plays a huge role in helping to regulate menstrual cramps. Your body goes through several changes every month and the kind of fuel you put into your body can affect your period pain. Eating the right food helps your body to deal more effectively with hormonal and physical changes.
Staying hydrated has a significant impact on your muscles and overall health. Ensure that you’re drinking enough water throughout the month.
Certain nutrients have proven to be especially useful when it comes to relief from pain. Try the following:
- Magnesium
- Vitamin B1 i.e. thiamine
- Vitamin E
- Pyridoxine
- Fish oil, either in the form of supplementation or by consuming fatty fish such as salmon
Start a better diet with our blog on Healthy Eating for Beginners. If you’d like expert advice, Avaana can help you find a nutritionist online.
Alternative forms of therapy for period pain relief
While there are a large number of alternative forms of therapy for dealing with menstrual cramps, there are some that are considered more effective than others.
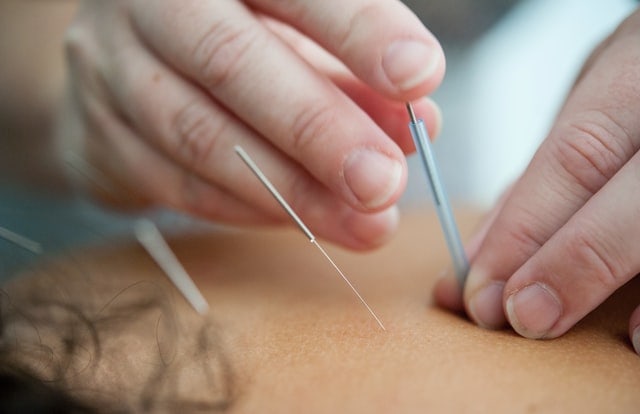
Acupuncture and acupressure manipulate various energy points in your body to relieve pain and enhance pain management.
Using an IUD for menstrual cramps
Many women use an intrauterine device as a contraceptive and have found that it has a successful impact on period pain relief.
The IUD is inserted into the uterus and can be kept there for up to five years. It releases a hormone called progestin which has several benefits, including reducing the intensity of menstrual cramps.
There are some things to remember before you decide to use an IUD:
An IUD will not protect you against sexually transmitted diseases; it is only meant to work as a contraceptive or for women who have extremely heavy or painful periods.
An IUD will be inserted by a medical expert after an examination. You will have to return to your clinic for checks or to have it removed.
An IUD may not be suitable for you if you have any conditions of the reproductive system including fibroids, or if you have certain forms of cancer, diabetes or blood pressure.